A Rutgers study examining how oncology doctors facilitate breast cancer patients’ psychological well-being has found that the use of more empathy by cancer care clinicians promotes better psychological health among patients.
“Our findings suggest that provider communication is a key component to reducing uncertainty, and thus providers play a key role in helping to facilitate psychological well-being,” said lead author SC&I Ph.D. Candidate Liesl Broadbridge. “Further, our findings are directly applicable as targets for communication training modules for health care providers, because by continuing to advance skills in empathic communication, clinicians can enhance the healthcare experiences of their patients.”
The study, “Facilitating psychological adjustment for breast cancer patients through empathic communication and uncertainty reduction”, was published in Patient Education and Counseling. In addition to Broadbridge, the authors are SC&I Professor of Communication Kathryn Greene; SC&I Associate Professor of Communication Maria Venetis; SC&I Ph.D. student Lauren Lee; SC&I alumna Smita C. Banerjee, Ph.D.’05, associate attending behavioral scientist at Memorial Sloan Kettering Cancer Center; Biren Saraiya, M.D., associate professor of Medicine, Division of Medical Oncology, and Section of Solid Tumor at Rutgers Robert Wood Johnson Medical School; and Katie A. Devine, Ph.D., associate professor of Pediatrics at the Rutgers Cancer Institute of New Jersey.
“Our findings suggest that provider communication is a key component to reducing uncertainty, and thus providers play a key role in helping to facilitate psychological well-being,” said lead author SC&I Ph.D. Candidate Liesl Broadbridge.
“Patients with breast cancer are at significant risk for developing symptoms of anxiety and depression related to their cancer diagnosis,” Broadbridge said. “As health communication researchers, we are interested in how health care providers can communicate in ways that help their patients cope with/manage their illness and support their psychological health.”
The research team, Broadbridge said, also investigated how the process of managing psychological well-being differs depending on whether the patients they surveyed were currently undergoing cancer treatment or had already completed their treatments.
Current and former patients experience different appointment types (i.e., treatment decision-making for current patients, watchful waiting for former patients), Broadbridge explained, and they therefore have had different lengths of time to adjust to diagnoses, and, potentially, have different relationships with their provider (i.e., more or less time to develop a relationship with the healthcare team).
“Although our findings were true for both current and former patients, the strength of the relationship between uncertainty and psychological adjustment was stronger for former patients than for current patients. This means that cancer care teams must continue to focus on uncertainty and issues regarding psychological health in cancer monitoring appointments and beyond the initial diagnosis/treatment phases of breast cancer survivorship,” Broadbridge said.
To conduct the study, the authors used online surveys to assess current and former breast cancer patients’ perceptions of their oncologists’ communication, the uncertainty they have about their diagnosis/treatment, and how they are coping with the illness.
“The findings of this study highlight the importance of both eliciting and addressing breast cancer patients’ uncertainty throughout the cancer trajectory to facilitate psychological adjustment,” Broadbridge said.
They recruited 121 current and 187 former breast cancer patients to participate in the study through the Love Research Army, a research registry hosted by the Dr. Susan Love Foundation for Breast Cancer Research, a national advocacy organization for breast cancer patients, survivors, and at-risk family members. The authors partnered with this community organization to broaden the sample of participants beyond the local New Brunswick area and to contribute to the larger conversations about cancer communication. The team also partnered with the Cancer Institute of New Jersey, with three of the study members (Broadbridge, Greene, and Devine) receiving grant funding to complete the project through the Cancer Survivorship and Outcomes Center Award.
“The findings of this study highlight the importance of both eliciting and addressing breast cancer patients’ uncertainty throughout the cancer trajectory to facilitate psychological adjustment,” Broadbridge said. “This is important because it underscores the role that clinicians play in helping patients manage both their physical and emotional/psychological health after breast cancer diagnosis.”
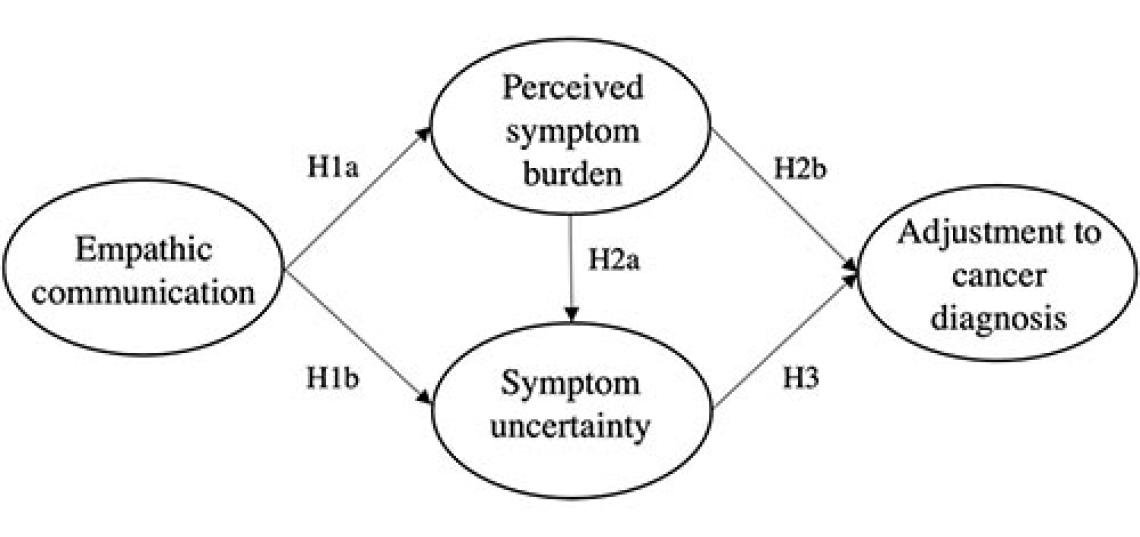
Image: “Fig. 1. Hypothesized psychological adjustment to uncertainty models” taken from the study, “Facilitating psychological adjustment for breast cancer patients through empathic communication and uncertainty reduction.”
Learn more about the Communication Department at the Rutgers School of Communication and Information on the website.
In the Media
US News & World Report: "A Doctor's Empathy Can Be Key to Breast Cancer Care."
Science Daily: “Empathetic cancer clinicians promote psychological well-being in breast cancer patients.”
Medical Net News: “Empathetic clinicians boost psychological health in breast cancer patients.”
Healthcare-In-Europe.com: “One of clinicians' mightiest weapons against breast cancer? Empathy.”
DoveMed: “Empathetic Cancer Clinicians Promote Psychological Well-Being In Breast Cancer Patients.”
